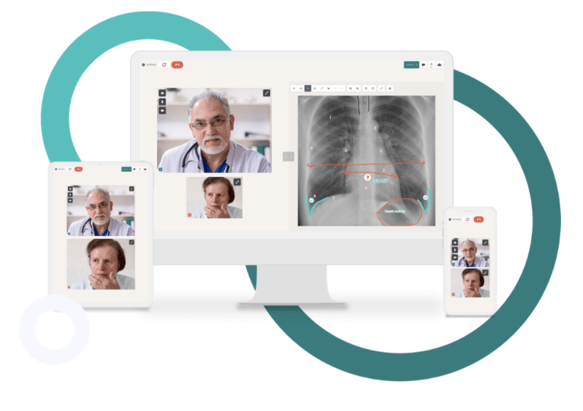
FAQs: The Clinical Aspects of Telehealth
Telehealth has been a hot topic this year, with traditional healthcare delivery models changing virtually overnight in the wake of the Coronavirus pandemic. But with this surge in telehealth usage, come many important questions about how to navigate this new blended model of healthcare. That is, offering both in-person consultations and video consultations.
On 18th November 2020, the Australasian Institute of Digital Health in partnership with Amazon Web Services held a facilitated panel on 'Clinical aspects of telehealth during COVID-19
CEO, Dr Silvia Pfeiffer was on the panel, along with GP and digital health advocate, Dr Andrew Baird and Child & Adolescent Psychiatrist, Dr Dave Carmody. There were too many questions from attendees to fit into the 1 hour webinar, so we have listed some general telehealth and Coviu related questions here, along with answers from Dr Silvia Pfeiffer.
- What strategies can be considered to assist the uptake of telehealth for elderly, hearing impairment and those with limited telehealth literacy or access to equipment?
Telehealth can include phone and video consultations, and also remote monitoring. Elderly people will mostly be challenged by modern technology, but in our experience, good training or accompaniment by a nurse or family member can overcome objections and complications.
For hearing impaired users, integration of phone and video technology with hearing implants is possible where sound from a computing device is directly transmitted via bluetooth to the implant.
Where people have limited access to technology or limited technical literacy, access via family members with technology or a community centre are options. At Coviu, we are soon releasing an add-on with Ezispeak, a language services provider, to deliver on-demand interpretation services during a Coviu video consultation. We are continuing to enter into these types of partnerships, to ensure barriers to telehealth access are addressed.
-
Are there still major telecommunication connectivity and capacity issues in supporting residents in rural and remote areas of Australia? If so, what are the hot spot areas that require advocacy at government level and what are the best avenues for such advocacy?
The NBN has seen widespread uptake, but there are still access challenges in certain areas. Telco companies continue to work to improve access where there are requests by users. The main thing to be done is for the user to request connectivity from their local providers or a telco.
NBN Co has a rollout map where you can check which addresses don't yet have access. Some very rural or remote areas will not be connected via fibre because of lack of population density or in fact for lack of population. Often, the only option in such places is Satellite for which capacity has been improved in recent years and should be available
I'm not sure if there's still a need to lobby the government - it's now in the hands of private companies to provide coverage. The extension of 5G networks will provide further coverage.
- From a clinical point of view, what evaluation have your teams undertaken around the outcomes of patients being seen via telehealth vs face-to-face?
A lot of research has been published about patient outcomes for telehealth in the last decade. That covers a vast diversity of services, from GPs to Allied Health, Specialist services as well as outpatient clinics in hospitals, aged care providers, and hospital in the home. Ongoing research is required, of course, since new technologies are continuously invented and with that, improved services will be available.
At Coviu, we have ourselves enabled our customers and research institutions to undertake patient outcome research on Coviu, being supportive via patient questionnaires post sessions, developing custom add-ons etc. As a vendor, we stay at arms length of such research so as not to be seen to influence it. Research has been published about Coviu in speech therapy and other research is under way in rehabilitation.
- How have you found Healthdirect works with the older less tech-savvy demographic?
In general, we have heard stories of elderly people getting quite used to the simplicity of access to clinics made available via the Healthdirect service. Once taught how to use it and given a device that is easy to use, they get quite comfortable with it. Occasionally you will find an elderly person who will object to learning new technology though - you can't win with everybody.
- Does Coviu allow clients to call in to a consult using their telephone while on the video consult? We have clients who don't have good data limits, or maybe they don't have a microphone on their computer.
Coviu doesn't yet have call-in functionality - it is something that's on our roadmap for next year. We have, however, developed call-out functionality, i.e. a clinician in a video call who is given the phone number of a patient can call them into an ongoing Coviu call.
Another option for the situation that you describe is also to get the patient on a Coviu call and after introductions, to turn off the video at both ends. Then it turns essentially into a phone call and doesn't use as much bandwidth. Video is the biggest consumer of bandwidth.
- Does Coviu allow us to have a custom subdomain for the meeting links?
Yes. When you sign up to Coviu, you get a custom subdomain of your choice at which your clinic is hosted. You can even change the colours in the Coviu consultation rooms to match your clinic's branding and you can add the logo of your practice so a patient will always know that they are entering your "virtual" clinic.
- Is there any resistance because of the use of patients' mobile data?
- How do you check for the vital signs in these telehealth tools?
A very good question! If vital signs need to be taken by a clinician, all they can do at the moment is to ask the patient to take these vital signs with any devices they might have available.
For example, temperature via a thermometer, a pulse rate via counting the pulse (by being directed how to get your pulse), and the rate of breathing by observing the patient via video. There are now also digital remote-monitoring tools that some patients have at home, which can measure vitals. Clinically validated Artificial Intelligence algorithms also continue to become available, that can calculate vitals via video analysis. It's definitely a space to watch, because there will be improvements in the coming year
- Digital recording of sessions is now possible. Is this a privacy concern?
At Coviu we make recording functionality optional. It requires consent to the recording by both the patient and the clinician, since private health information is being recorded and thus creates ePHI which falls under regulation. Most clinicians are hesitant to be recorded since they are afraid that their knowledge and practice will be under more scrutiny. It turns out though that indemnity insurances actually like the idea of telehealth and even more the idea of recordings because it, in general, protects clinicians from malpractice suits.
In addition, a recording can be used to give patients better information, since they can take the recording home and replay it at their leisure to review the instructions by the practitioner. From a privacy point of view, if the patient has a recording, they have to make sure to keep their own data safe. Practitioners have to handle the data carefully - it's best stored in encrypted form with limited access to the recording, at the clinic at which the consultation was held.
- Out of curiosity - did local PHNs provide telehealth education and support?
At Coviu we are aware that Healthdirect has educated PHNs about the use of telehealth, and in turn, PHNs have offered education to their clinics. Not all clinics have taken up this opportunity, and not all might have been aware that this opportunity was available. There is also training available from industry associations and many other online courses. At Coviu we are offering a lot of training material and some courses also.
- Please comment on the usefulness of My Health Record.
In my personal opinion, My Health Record does not yet store enough of my own personal health information. I'd wish it to be the central storage of all information about my health history so I wouldn't need to explain my history to any practitioner that I have dealings with.
However, right now, it only stores a limited set of data. That is, however, a start and I have to believe it will improve over time. I've heard of patient cases where the access to MyHR has saved patients' lives. That is the results I'd like to see, plus improvements to the quality of care because everyone in my care team has full visibility of my medical history as a patient. We're definitely not there yet though.
- How do you manage the money/billing transactions?
Coviu offers a Credit Card payment functionality and has just released our integration with Medipass for Medicare, private healthcare and other types of reimbursements. The idea is to make Coviu as simple as possible to support the full interaction between the patient, the practitioner and the practice manager, including the financial transactions.
- There are diverse views from practitioners on tools to use for telehealth e.g. Facetime, Skype, Zoom (free) and even when security standards are invoked, a dependency on HIPPA compliance. What actions are being taken to help the Australian healthcare providers understand what telehealth standards actually relate to them for data processing, data storage, security etc?
Healthcare practitioners receive such information from their industry associations. We have observed during the crisis that all industry associations have updated their website and training material around telehealth to support their members.
For example, the RACGP has extensive information about what is an appropriate telehealth consultation and what tools are acceptable to use. However, we have seen different industry associations pick different recommendations for their practitioners and give diverging advice - some recommending the use of consumer tools for clinical use.
We believe that is not appropriate - purpose-built tools should always be preferable since they come with privacy and security built in, and with appropriate workflows and clinical tools. It is indeed still something that is a work in progress, to provide minimum quality standards for Australia. In the US, consumer tools are not acceptable for clinical use.